The 2020 Instructions for Forms 1094-C and 1095-C
reading time: 10 minute(s)
As the end of 2020 draws near, it’s time for employers to out together a game plan for their 2020 ACA reporting. The first step is understanding the changes to the revised Forms 1094-C and 1095-C, because these changes could affect what information you are reporting to the IRS.
Most of the changes to these forms are in reference to the Individual Coverage Health Reimbursement Arrangement, or ICHRA. This type of health insurance coverage plan is now allowed under the Affordable Care Act (ACA).
Here is a guide to navigating the changes to these forms.
What is an ICHRA?
An ICHRA, or Individual Coverage Health Reimbursement Arrangement, is an alternative for traditional health insurance group plans. With this type of plan employees choose their own health insurance coverage, potentially from the Healthcare Marketplace. Because their employer receives a tax deduction for these plans, their employees in turn get a tax-free reimbursement.
The employee is initially responsible for the monthly premium and medical expenses related to the plan. Then after submitting the required information to their employer, they will receive set reimbursements.
As of January 1, 2020, employers are now able to offer the ICHRA to their employees.
As you will see many of the changes to the Form 1095-C are based around the inclusion of the ICHRA in ACA 1095 reporting.
What is the Form 1094-C?
This is the Transmittal of Employer-Provided Health Insurance Offer and Coverage Information Returns. This is a long name for a short form. The Form 1094-C the authoritative transmittal, in other words it is basically a cover page for the IRS Form 1095-C that briefly summarizes the information within these forms.
Whether you are paper mailing your forms or e-filing them, you will need to attach this form. It provides information about how many forms you are sending, your contact information, and your business information.
This good news is that this form has essentially remained the same for the 2020 tax year.
What is the Form 1095-C?
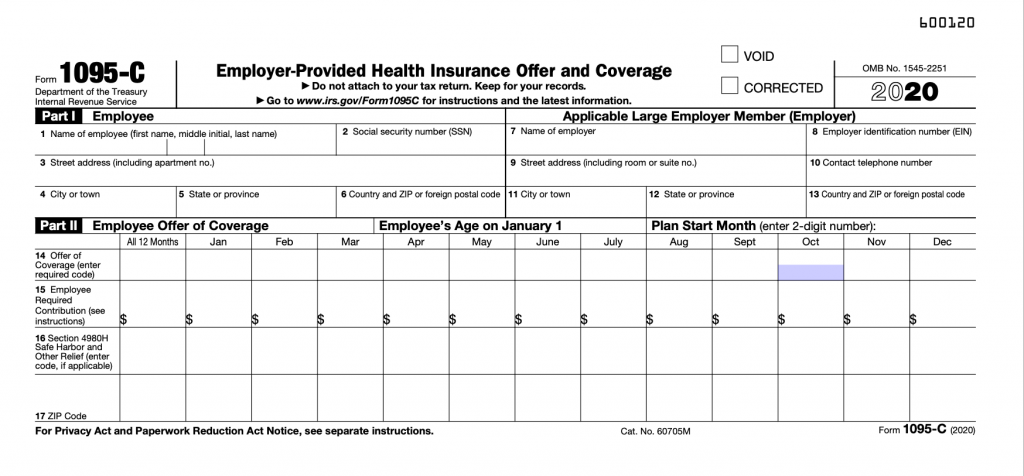
The Form 1095-C is the Employer-Provided Health Insurance Offer and Coverage. IRS Form 1095-C is designed by the IRS to capture enough information about the employer’s offer of health insurance coverage and to verify that these employers are in fact meeting the requirements for minimum essential coverage.
Applicable Large Employers (ALEs) with 50 or more full-time or full-time equivalent employees are required to file Form 1095-C.
What are the changes to Form 1095-C for 2020?
There are specific changes to the Form 1095-C to reflect the reporting of ICHRAs. First, there is an entirely new line that captures the employee’s zip code, Line 17.
This line indicates the zip code of the employee. This will be used to determine affordability. This applies to employees who were offered an HRA by their employer.
Employers will also need to include the Plan Start Month for each employee. This change applies to all plans, not just the ICHRA. For ICHRA plans, the age of the employee at the start of their plan must be included as well.
In addition to this, there is an entirely new set of ACA codes (Code 1L -1S) that refer to the ICHRA coverage.
Click here to learn more about Form 1095-C Codes.
Are you ready to begin e-filing Forms 1094-C and 1095-C?
If you have all the information you need to file your Form 1095-C and Form 1094-C, you can easily e-file them using TaxBandits before the Form 1095-C deadline. You can use our bulk upload feature to save time and skip manually entering your data.
To get started today, simply create your free TaxBandits account!


Leave a Comment